Understanding the Persistent Cough
You wake up every morning knowing that first cough is coming. It's not just a cold that won't go away; it's Chronic Bronchitis, which is a type of long-term inflammation affecting your airways characterized by a productive cough lasting at least three months over two consecutive years. Unlike acute bronchitis, which clears up in weeks, this condition sticks around. About 75% of cases link directly to smoking history, making it one of the major faces of Chronic Obstructive Pulmonary Disease (COPD). While statistics show it ranks as the fourth leading cause of death in places like the United States, understanding exactly what's happening inside your chest changes how you deal with it day-to-day.
The Role of Mucus and Airflow
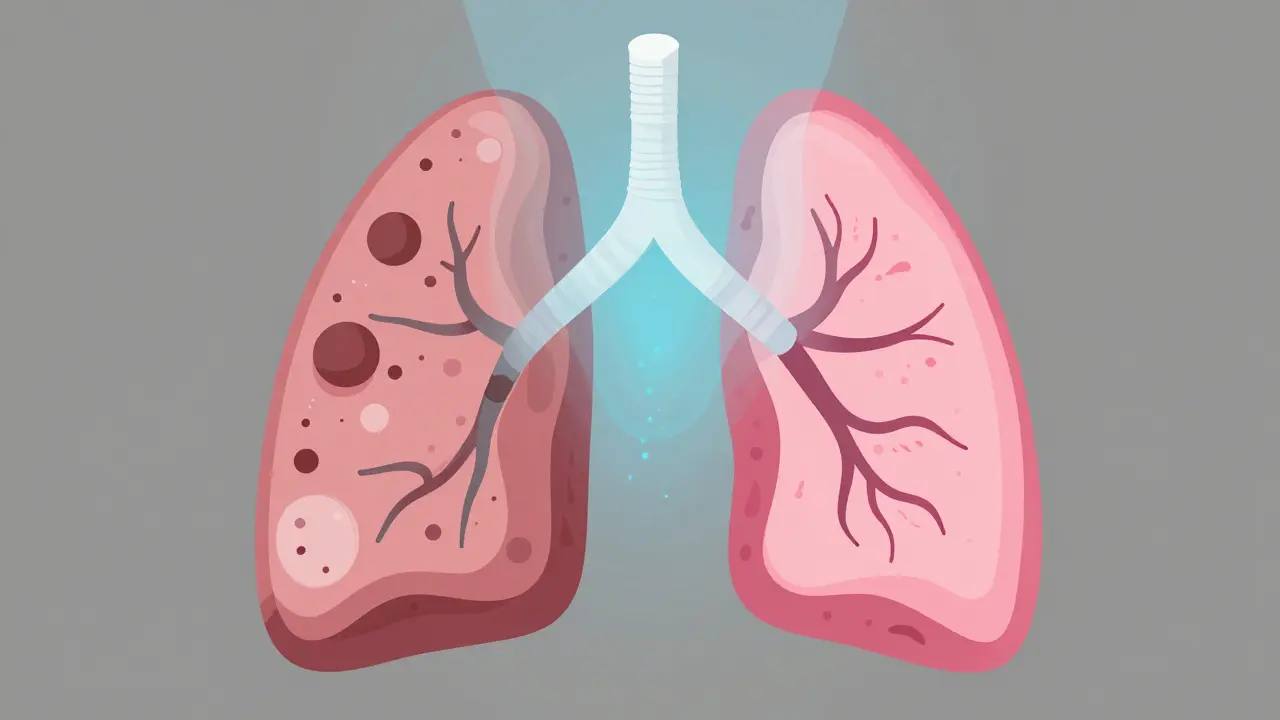
Your lungs usually handle debris quietly, but when Chronic Bronchitis takes hold, the lining of the bronchial tubes gets irritated. This irritation triggers your body to make too much mucus. Think of it like a factory working overtime to protect the system, but the protection becomes the problem. You produce significant sputum because your body tries to trap dust, smoke, and bacteria in sticky fluid. When airflow is blocked by this congestion, you feel tightness in your chest. Studies from UCSF Health note that 68% of patients report this chest tightness as moderate to severe. The blockage forces you to breathe harder, leading to shortness of breath during simple tasks like walking or climbing stairs. Roughly 82% of patients experience this breathlessness specifically during exertion.
Why Quitting Smoking Changes Everything
If you are still lighting up, the numbers don't lie. Over 90% of people with chronic bronchitis have a smoking history. However, Smoking Cessationrefers to the process of stopping tobacco use completely to allow lung tissue repair and prevent further decline remains the single most effective intervention available. It isn't just about slowing down the damage; it's about survival. Medical authorities agree that quitting stops the progression of the disease faster than any drug currently exists. Dr. John Walsh from the COPD Foundation highlighted that quit rates above 50% correlate with 60% slower disease progression compared to continuing smokers. Even if you've smoked for decades, removing the irritant allows your cilia-the tiny hairs cleaning your lungs-to start working again.
Making Stopping Work for You
Trying to quit on your own often fails because the addiction is chemical and behavioral. Structured support changes the odds significantly. A survey found 68% of patients who received professional support successfully quit, versus only 22% who tried alone. Effective programs combine medication with counseling. Varenicline paired with nicotine replacement therapy offers high success rates. When these methods integrate with behavioral strategies, abstinence rates hit 45% at six months. Without help, the spontaneous quit rate drops to nearly 7%. This gap shows why relying on willpower alone is risky for someone with compromised lungs.
Treatment Options Beyond Quitsmoking
Once you address the smoking habit, you need tools to manage the daily symptoms. There is no cure for chronic bronchitis, but comprehensive management improves quality of life drastically. Doctors follow guidelines like the 2023 GOLD guidelines to decide the right mix. Below is a breakdown of common interventions:
| Intervention Type | Primary Goal | Efficacy / Outcome | Potential Side Effects |
|---|---|---|---|
| Bronchodilators | Open air passages | Relief within 15 minutes (Short-acting) | Rapid heart rate, tremors |
| Inhaled Steroids | Reduce inflammation | Symptom relief over weeks | Osteoporosis risk, hypertension |
| Pulmonary Rehabilitation | Improve endurance | Walk distance +78 meters average | Physical fatigue initially |
| Antibiotics | Treat bacterial infection | 82% efficacy for bacterial exacerbations | Digestive upset, resistance |
Many patients struggle with complex regimens. On forums like Reddit, users often mention difficulty coordinating multiple inhaler techniques. Proper technique is critical because 38% of patients need more instruction than initial training provides. Working with a respiratory therapist ensures the medicine actually reaches your lungs instead of your throat.

Living with the Condition Long-Term
Staying healthy involves protecting your immune system. You are 3.2 times more likely to catch viral and bacterial infections than the general population. Annual influenza vaccination reduces exacerbation risk by 42%, according to CDC data. Pneumococcal vaccination every five to seven years provides protection against pneumonia complications. These aren't optional extras; they are part of the core defense plan.
For some, oxygen becomes necessary. If blood oxygen saturation falls below 88%, continuous oxygen therapy helps. Data shows using oxygen for 15+ hours a day increases 5-year survival by 21%. Compliance is hard-only 62% stick to the prescription-but the impact on longevity is real.
What Success Looks Like
Success isn't just about living longer; it's about doing things again. Patient communities show that 78% report symptom improvement after rehab programs. One former smoker reported walking to the end of his street without stopping after six months of consistent work. Another noted improved ability for daily activities. However, side effects can happen. Some patients face issues with steroid inhalers causing bone density loss. Monitoring is essential so doctors can switch therapies if risks outweigh benefits.
Looking Ahead
New treatments are emerging. In May 2023, FDA approved ensifentrine, a phosphodiesterase inhibitor showing a 15% reduction in exacerbations. Research into gene variants related to mucus clearance might enable personalized mucolytic therapy soon. Digital tools, like AI-powered inhaler sensors, promise to increase adherence by tracking usage accurately. Regardless of the gadgets or drugs, the foundation remains the same: stop the smoke, move your body, and protect your lungs from infections.
Can chronic bronchitis be cured completely?
There is currently no permanent cure for chronic bronchitis. However, effective management strategies can slow disease progression, reduce symptoms, and significantly improve your quality of life.
How does smoking affect my diagnosis timeline?
Quitting smoking immediately slows the rate at which lung function declines. Statistics show that quitting results in 60% slower disease progression compared to continued smoking.
Is pulmonary rehabilitation safe for me?
Yes, it is generally considered standard care. Programs include education and exercise tailored to your level, improving walk distance by an average of 78 meters for participants.
Do I really need flu shots every year?
Absolutely. Influenza vaccination reduces the risk of exacerbations by 42%. Since your lungs are vulnerable, preventing respiratory infections is crucial for stability.
When should I worry about sputum color?
If your sputum turns yellow or green and you feel worse, it may signal a bacterial infection. Contact your doctor immediately, as antibiotics like amoxicillin-clavulanate have shown 82% efficacy in these cases.

Victor Ortiz
March 31, 2026 AT 08:40The data presented here is fairly standard for anyone following COPD literature closely. Statistical correlations between smoking history and disease progression are well established. There is little room for debate on the efficacy of cessation programs versus willpower alone. Most patients underestimate the chemical dependency involved in nicotine addiction. Behavioral counseling works significantly better than isolation approaches. Ignoring the medical guidelines leads to worse outcomes consistently.
Carolyn Kask
April 1, 2026 AT 12:46You sound like everyone else who thinks numbers tell the whole story. Statistics rarely account for individual resilience factors. Our healthcare system already prioritizes prevention over treatment costs. I suggest looking at the actual implementation rather than theoretical efficacy rates. People ignore the financial burden of these therapies entirely. It is not just about biology but logistics too. Keep trying to simplify complex medical reality into bullet points though.
Amber Armstrong
April 2, 2026 AT 14:23I remember watching my grandfather cough through entire movie nights. It was always hard hearing him struggle to catch his breath. He never complained but you could see the pain in his face. We thought it was just old age until the doctor finally explained things. Turning out to be chronic bronchitis changed how we treated him at home. Keeping the house clean became a full-time mission for our family members. Dust seemed to trigger bad episodes more than anything else did. He tried quitting smoking several times over the course of decades. Withdrawal made him irritable and constantly tired during the process. Eventually he found a clinic that helped him through the worst parts. Support groups were essential for him to feel less isolated in life. Medicine is advancing but lifestyle changes still remain crucial for survival. Seeing these statistics reminds me why consistency matters so much now. Every small improvement adds up to quality time with loved ones later. Please take care of yourselves if you are reading this story tonight. You deserve to find peace even when the lungs are fighting.
Brian Yap
April 4, 2026 AT 07:03G'day mate, that is a really touching story there. Sounds like your grandad was a tough bloke. Hope it helps others here realize they are not alone in this mess.
Katie Riston
April 5, 2026 AT 08:54We often forget the philosophical weight of breathing as a daily act. Air becomes something we fight for rather than something we inhabit. The transition from healthy to ill shifts one's relationship with time itself. Symptoms become the clock ticks counting down vitality. Yet there is dignity in managing the decline with purpose. Acceptance does not mean giving up but changing the battlefields.
Ruth Wambui
April 6, 2026 AT 22:50Notice how the big pharmaceutical push relies on keeping you medicated forever. Why stop smoking if they sell inhalers for a lifetime? The air quality warnings are convenient excuses for prescription refills. Natural cilia recovery gets ignored to protect revenue streams. They want us dependent on pumps instead of fixing the root cause.
Michael Kinkoph
April 7, 2026 AT 21:07Indeed!; however!; one must; understand; the nuance! While skepticism is healthy!; blind denial of modern medicine!; endangers lives! Clinical trials!; provide evidence!; unlike vague accusations! Regarding systemic corruption!; we must prioritize patient safety!; over baseless theories!
Jonathan Sanders
April 9, 2026 AT 17:42This is exactly how I feel every single day without fail.